Different Types of Colorectal Tests
The colon and rectum are two integral components of your digestive tract. They bear the critical responsibility of both processing and eliminating waste products.
Should either of these parts of your large intestine sustain damage or disease, digestive processes can be hindered, which can have a serious impact on your well-being and longevity.
Gastroenterologists have many colorectal tests at their disposal to detect problems existing in these regions.
Reasons a Doctor Might Order a Specific Test
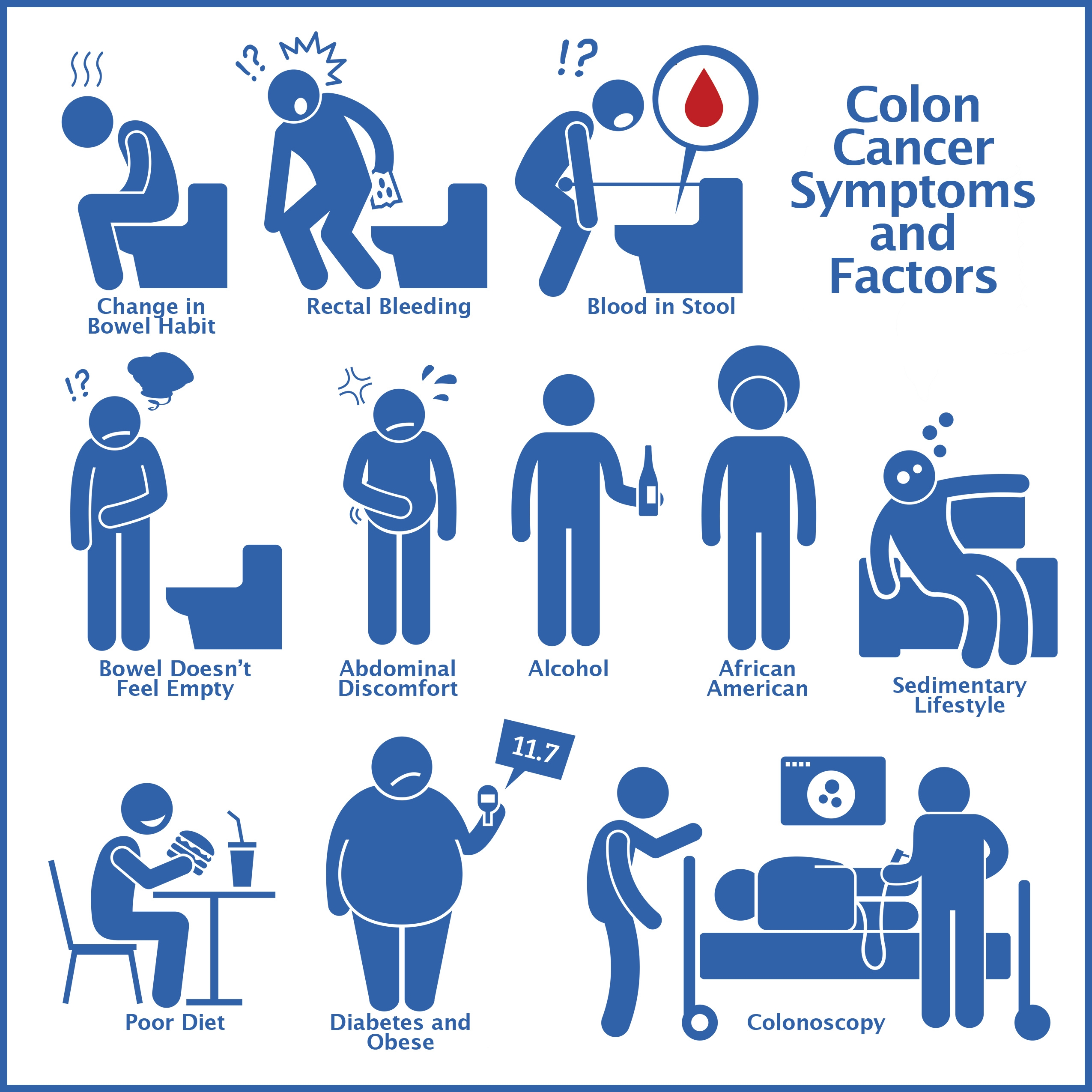
Your physicians will likely use a diagnostic test like a colonoscopy if you have long-standing or serious symptoms, including:
- Blood in the stool.
- Persistent or moderate to severe abdominal pain.
- Active bleeding from the anus.
- Chronic or severe bloating.
- Frequent constipation or diarrhea.
- Appetite loss.
- Unexplained or unintended weight drops.
Your doctor might choose to administer such tests even when you are don’t show symptoms. They can detect potentially dangerous problems like colon polyps and are used if you are over a certain age. Your risk of developing colon and rectal malignancies increases significantly as your reach middle and older ages.
Conditions Colorectal Tests May Help Diagnose
You might think these detection efforts are only used to diagnose cancer. While the identification of colon and rectal malignancies is the primary aim of the different colorectal tests, they are also employed to identify other maladies, such as inflammatory bowel disorders like Crohn’s Disease and ulcerative colitis, benign growths, infections, and internal bleeding.
The Different Types of Colorectal Tests
These diagnostic tools usually fall into three categories: internal imaging examinations, stool samples, and biopsies.
Internal Imaging Tests
Doctors use various apparatuses to capture internal images of your colon and rectum. Some of the more commonly used procedures include colonoscopies, abdominal X-Rays, and MRIs (Magnetic Resonance Imaging).
Colonoscopies
Arguably, the most utilized colon-examination tool is a colonoscopy.
Overview
This test is performed using an elongated, thin, camera-equipped tube known as a colonoscope, which your doctor uses to examine the organ, identify problematic areas, and confirm a specific diagnosis.
Preparation
This test is relatively easy and painless, but you will be required to prepare for it properly.
The most critical action is to ensure that your colon is clear. Any lingering material can interfere with administration or skew the results. You might be asked to avoid solid foods and consume only clear liquids preceding the exam, use laxatives to speed up the elimination of your colon’s contents and adjust your usage of any blood-thinning or blood-impacting medications. Your physician will give you specific instructions.
The Procedure
You will be sedated before administration. When the test is ready to begin, the performing physician will lie you down on an examining table and carefully insert the colonoscope through your anus and into your rectum.
As the tube probes further, air is pumped into your colon to enlarge the organ and render it easier to view. Once the apparatus arrives in your colon, your doctor will examine the images the camera captures on a computer screen.
Recovery
The process lasts anywhere from 30 minutes to a full hour. You will need someone to drive you home or arrange some other form of transportation because you will still be groggy from the sedative and unable to operate a motor vehicle.
You might experience minor, short-lived symptoms, such as gas, bloating, slight discomfort, and difficulty walking. It is not abnormal to pass a tiny amount of blood for a day or two following the event. If any of these symptoms linger or intensify, notify your doctor immediately.
Abdominal X-Ray
Overview
Using fluoroscopy, physicians can capture X-Rays of your colorectal region. This specific test is called a lower GI series because the large intestine is considered part of your lower gastrointestinal system.
Preparation
Your doctor will provide specific instructions. You are advised to follow a low-fiber diet for the two to three days preceding the test and not smoke or ingest certain drugs the day before administration. You will likely be asked to undergo an enema or use laxatives to clear out your digestive tract ahead of the examination.
The Procedure
You will be placed on an examining table where a physician or technician will administer a barium enema. Barium is an illuminating substance that lights up on X-Ray screens, enabling examining physicians to see any problematic issues. Your doctor might ask you to move around during the exam, to keep the liquid preparation flowing properly.
In many instances, several sets of X-Rays are taken. This means the barium administration process may be repeated. Usually, the entire procedure takes no longer than a half-hour to 60 minutes.
Recovery
Typically, you can return to normal activities and a regular diet immediately following the test. You should drink additional fluids to ensure the barium contents are promptly eliminated from your system.
Magnetic Resonance Imaging
This diagnostic effort, often abbreviated as an MRI, uses magnets and radio waves to capture internal bodily images of organs like the large intestine.
Preparation
In most instances, you will not be held to any dietary restrictions before an MRI. But you will need to:
- Remove any body piercings.
- Remove all jewelry.
- Notify your doctor if you have any metal implants.
- Be honest about your medical history.
Above all, you should follow whatever instructions your doctor offers. Failing to do so could delay administration or produce flawed findings.
The Procedure
After removing jewelry and other items such as your glasses and any other items containing metal, you will be fitted on to a sliding table. An MRI machine is an elongated tube you slide into. The machine emits noise as it captures scans. If you are sensitive to loud noises, you may be given earplugs or headphones to mitigate associated discomfort.
Recovery
If you need sedation to offset claustrophobic fears, you will need to secure transportation home because the drugs will adversely impact your capacity to drive.
Stool Samples
The colon and rectum respectively produce and expel the solid waste product called stool. Because this material is created and passes through those regions, doctors often study its contents to determine the presence of illness or injury. These are called stool samples.
Overview
There are three types of stool exams commonly performed. The guaiac-based fecal occult blood test, often abbreviated as gFOBT, the fecal immunochemical test, often shortened to FIT, and the FIT-DNA examination.
The Fecal Occult Blood Test
The fecal occult blood test is used to detect hidden (occult) blood in the stool. Occult blood is usually passed in such small amounts that it can be only detected only through the chemicals used the test.
The test can indicate colon cancer or polyps in the colon or rectum, but not all cancers or polyps bleed. Also, the fecal occult blood test can’t determine what’s causing the bleeding. It can only detect the presence or absence of blood.
Additional tests are needed to determine the source of the bleeding if blood is detected through the test.
To perform this test, you are given an administration kit containing a stick or brush. You will use the kit to collect a small concentration of your stool, place it inside the kit, and return it for further investigation. A chemical called guaiac is administered to detect small, hidden amounts of blood in the stool.
A fecal occult blood test isn’t recommended if you notice blood in your stool, or in the toilet or if you experience abdominal pain or a change in your bowel habits.
The Fecal Immunochemical Test (FIT)
This test uses antibodies to search for blood’s presence in stools. The administration and examination formats are like those seen with the fecal occult blood test. If the results come back positive for blood in the stool from a FIT test, your doctor will want to perform other tests, usually including a colonoscopy.
The FIT-DNA Test
This test searches for blood, in addition to altered samples of DNA inside stools. For this test, you collect a full bowel movement and transfer the sample to a laboratory for additional study. Cologuard® is a FIT-Fecal DNA test.
Colon Biopsies
A small portion of colon tissue is extracted from your body during a biopsy and sent to a lab for further assessment.
Colon biopsies can be performed during a colonoscopy. A colonoscope contains a tiny knife to collect tissue samples. Therefore, the preparation, procedure, and recovery for colon biopsies are like colonoscopies’ protocols.
Contact Us
Learning you need to undergo further testing for a potentially serious colon or rectal disorder can be a frightening and trying experience.
Our practice began more than 15 years ago and has emerged as one of the leading gastroenterology practices in central Florida. We perform a host of diagnostic procedures using state-of-the-art equipment in a friendly, comfortable, and inviting atmosphere where patient care is always a top priority. Contact us today!