What Are Polyps and How Are They Treated?
The colon is a large and critical organ found in your digestive tract. It executes several life-sustaining functions.
Unfortunately, many ailments can negatively impact the colon’s structure and operability. One such issue is known as polyps. Different types of colorectal tests are available to help doctors detect and treat colon polyps.
Overview
Polyps are formations of cells accumulating along your colon’s lining. Doctors place polyps into two primary categories: non-neoplastic and neoplastic.
- Non-Neoplastic Polyps – This variation is typically the most harmless and does not eventually turn cancerous. Sub-categories of non-neoplastic polyps include inflammatory, hamartomatous, and hyperplastic.
- Neoplastic Polyps – These growths can ultimately morph into malignant tumors. Major sub-categories of neoplastic polyps include serrated and adenomas.
Causes
Researchers have not yet discovered one specific cause. Colon polyps may result from a combination of genetic and lifestyle factors, such as:
- Consuming large amounts of red meat and foods with significant fat concentrations.
- Eating minimal quantities of fiber.
- Being obese.
- Smoking cigarettes or using other tobacco products.
- Excessive amounts of alcohol.
Medical professionals also believe genetic flaws might cause colon polyps.
Risk Factors
Your risk of developing colon polyps increases if you are:
- Age 50 And Older – Colon polyps most commonly occur in individuals 50 and older.
- African American – Colon polyps are most prevalent in African Americans. Polyps developing in persons in this ethnic group are more likely to turn cancerous.
- Have A Family History of Colon or Bowel Disease – People with a family history of colon polyps are more likely to develop the condition. Your chances increase if you have been diagnosed with an inflammatory bowel disorder like Crohn’s Disease or ulcerative colitis.
- Have Diabetes – Your probability increases if you have Type Two diabetes. The chances rise even further if the condition is not managed correctly.

Symptoms
Occasionally, colon polyps do not produce any symptoms. But common symptoms include:
- Rectal Bleeding – Colon polyps may result in rectal bleeding. The rectum is located at the lower end of your colon and helps the body process and expel the waste product known as stool. Sometimes, blood passes with stool and can be seen inside fecal material. On other occasions, concentrations are so small that they are only detectable under laboratory-grade microscopes.
- Anemia – This potentially serious medical condition occurs when your red blood cell count is abnormally low. Anemia commonly impacts persons with minor and gradual blood loss. Symptoms include extreme tiredness, weakness, coldness, breathing difficulties, and dizziness.
- Bowel Movement Irregularities – Colon polyps can render passing bowel movements more challenging. In addition, bouts of constipation or diarrhea are not uncommon. The size, shape, and texture of such waste products might change.
- Depleted Systemic Iron Concentrations – Doctors also report diagnosing iron deficiencies in individuals with colon polyps.

Complications
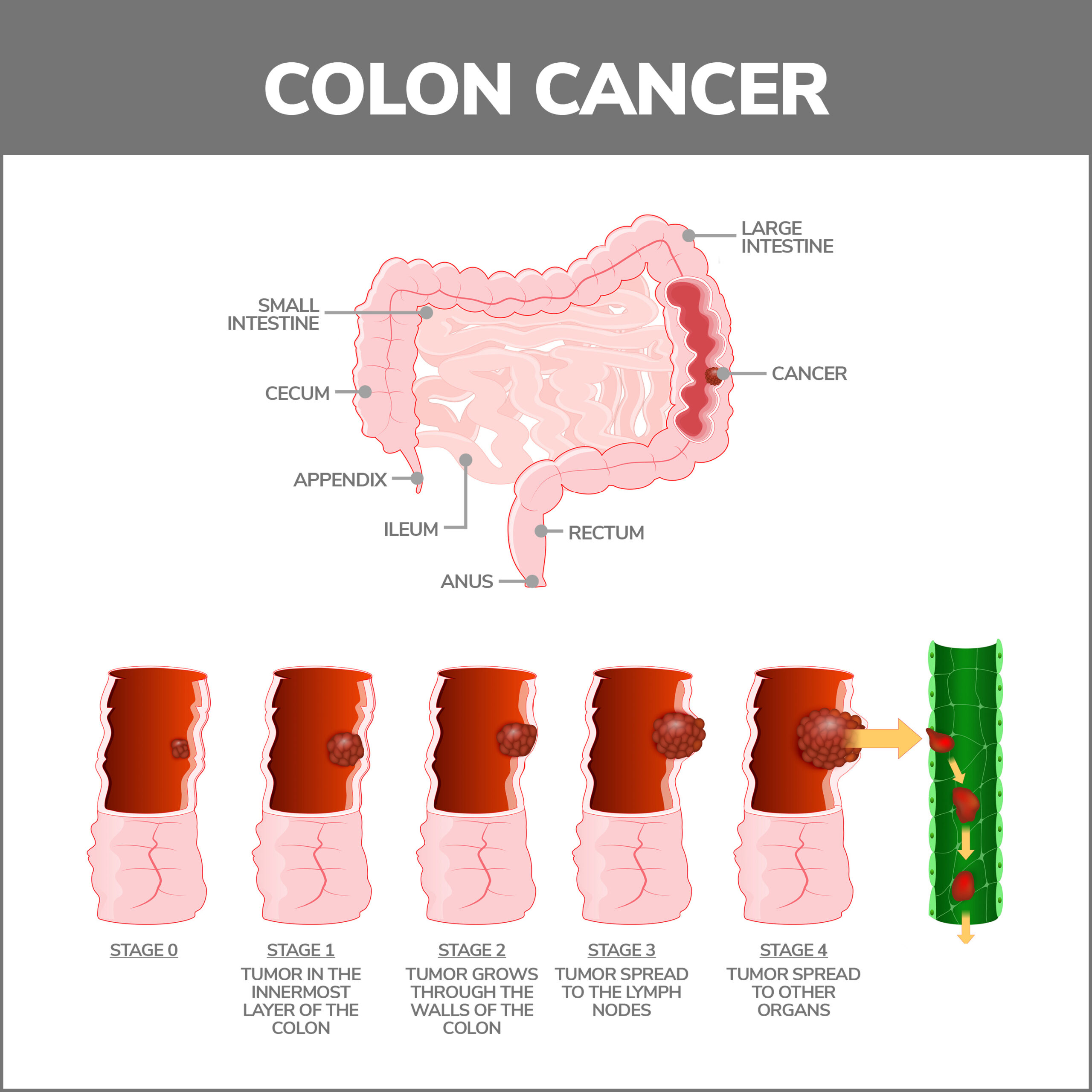
Large polyps can result in serious complications such as bleeding, bowel obstruction, and many digestive issues.
The most significant possible complication is cancer. Researchers caution that an appreciable percentage of more significant neoplastic masses eventually turn malignant. Colon cancer claims many people’s lives because it is not always diagnosed at an early and more manageable stage.
Diagnosis
Different types of colorectal tests aid physicians in the diagnosis of colon polyps. Such examinations include:
- Computerized Tomography – A CT scan is a diagnostic test that lets doctors capture internal images of your colon.
- Stool Samples – These tests identify the presence of blood or any other stool irregularities. Abnormal stools may show the presence of polyps or cancer.
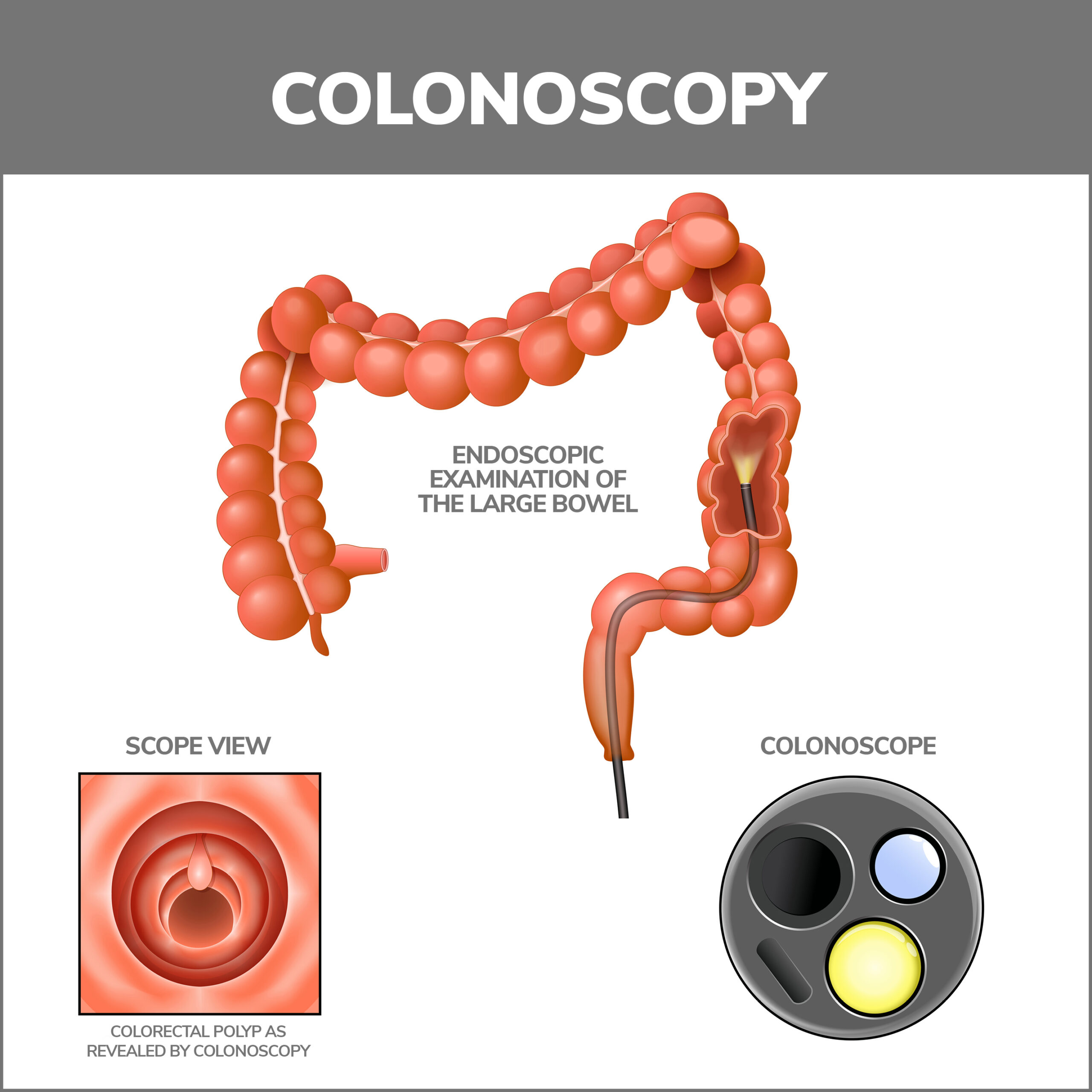
- Colonoscopy – During this commonly performed procedure, doctors insert an elongated tube fitted with a camera through your rectum and into your colon. The camera produces photos of your colon that doctors can use to detect anomalies like polyps.
- Sigmoidoscopy – Similar to a colonoscopy, physicians insert a tube-like, camera-equipped device known as a sigmoidoscope into your rectum to study the sigmoid colon. Unlike a full colonoscopy, this test only checks the lower part of your colon (the sigmoid colon.)
Treatment Options
Polyp removal is the preferred treatment. Polyps can be removed during colonoscopy or sigmoidoscopy procedures. These devices are also fitted with tools capable of cutting the growths away. In medical terms, this process is called a polypectomy. Open surgery might be indicated to remove especially large masses or numerous polyps.
Prognosis
Prognosis you will make a full recovery following the removal of uncomplicated polyps. But polyps tend to recur. You should schedule routine screenings and display added vigilance if you have a family history of colon cancer or any other type of malignancy.
Prevention
Polyp growth cannot always be prevented. This is especially true if the masses result from a genetic predisposition.
Specific preventative efforts include:
- Consuming A Healthy Diet – You may lower your risk by eating a high-fiber diet. Fiber plays a vital role in ensuring digestion runs quickly and efficiently. Food containing large quantities of fiber includes fruits, vegetables, and grain products like cereal, peas, and lentils. Avoid highly processed foods, red meat, and edible items containing notable fat concentrations.
- Shedding Excess Pounds – Grossly overweight or obese people stand at greater risk. They are strongly encouraged to lose weight through efforts such as exercising, limiting caloric intake, and remaining adequately hydrated.
- Limiting Stress – Overly-stressed individuals tend to eat more fatty and processed foods. Anxiety often stimulates the stomach’s production of acid. This substance can irritate the colon’s lining, increasing your susceptibility to various digestive system problems. It may exacerbate symptoms caused by polyps.
- Augmenting Your Diet Using Vitamin Supplements – Nutrition-related studies have shown that nutrients like Vitamin D and calcium enhance colon health and may decrease your risk of developing polyps.
- Eliminating Questionable Lifestyle Vices – Quit smoking and drinking. Tobacco products and alcoholic beverages contain chemicals known to inflame your digestive tract’s lining.
- Using Aspirin Regularly – Taking small dosages of aspirin. Studies conducted revealed that this practice may keep polyps from turning malignant. Speak with your doctor before beginning any type of aspirin-related therapeutic regimen. This is particularly true if you have digestive tract ulcers or any other medical condition known to cause bleeding.
- Obtaining Regular Medical Checkups – Everyone over 50 is encouraged to undergo colon cancer screening. If you are African American, have been diagnosed with an inflammatory bowel disorder, or have a family history of cancer, the process should begin at age 45.
Seek medical evaluation should any polyp-related symptoms occur. It cannot be overstated that any identifiable problem is easier to remediate in its earliest stages.
Reaching Out to Us
Please schedule a consultation if you are concerned about this condition or believe you may have it. Our practice began more than 15 years ago and has emerged as one of the leading gastroenterology practices in central Florida. We perform a host of diagnostic procedures using state-of-the-art equipment in a friendly, comfortable, and inviting atmosphere where patient care is always a top priority. Contact us today!