
Esophageal Disorders
Your esophagus is one of your digestive system’s major components. Disorders can potentially cause troublesome symptoms and sometimes life-threatening problems.
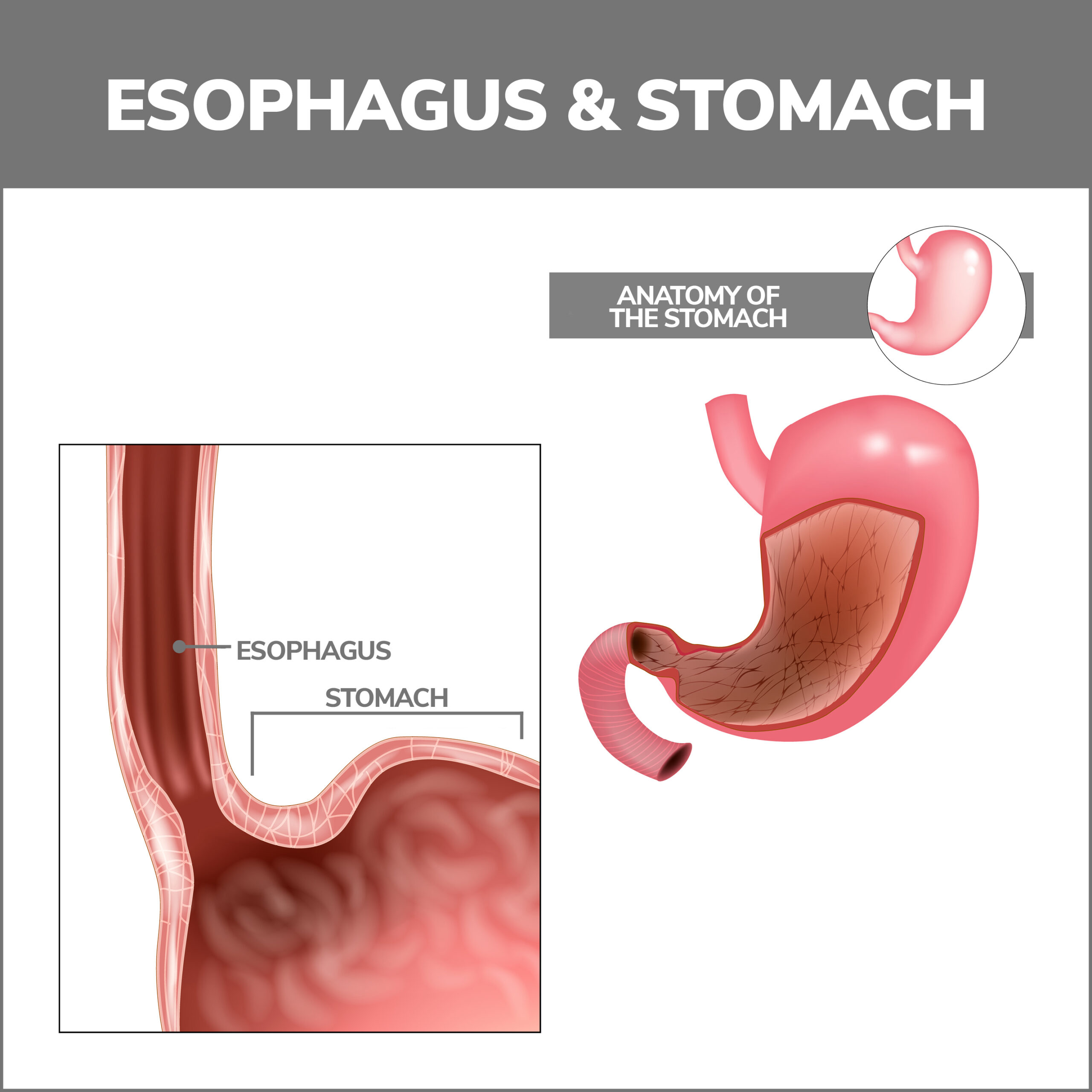
Esophagus Overview
The esophagus is a tube-like structure connecting your throat and stomach. It begins digestion by transporting food and beverages you consume from your mouth to your stomach.
The esophagus has two primary components: the upper and lower esophageal sphincters. The upper section is located close to your throat. The lower region lies next to the stomach. These sphincters are muscles that open when you eat and close during the esophagus’s idle periods.
Common Types of Esophageal Disorders
Several different ailments can affect the esophagus’s structure and function. Common examples include:
- Esophageal Narrowing – Over time, the esophagus’s pathway grows narrow. Such events render swallowing difficult and could inhibit digestion.
- Esophagitis – Upper respiratory issues and nasal allergies can result in the accumulation of white blood cells (eosinophils) inside your esophagus. This can lead to inflammation of the organ’s lining.
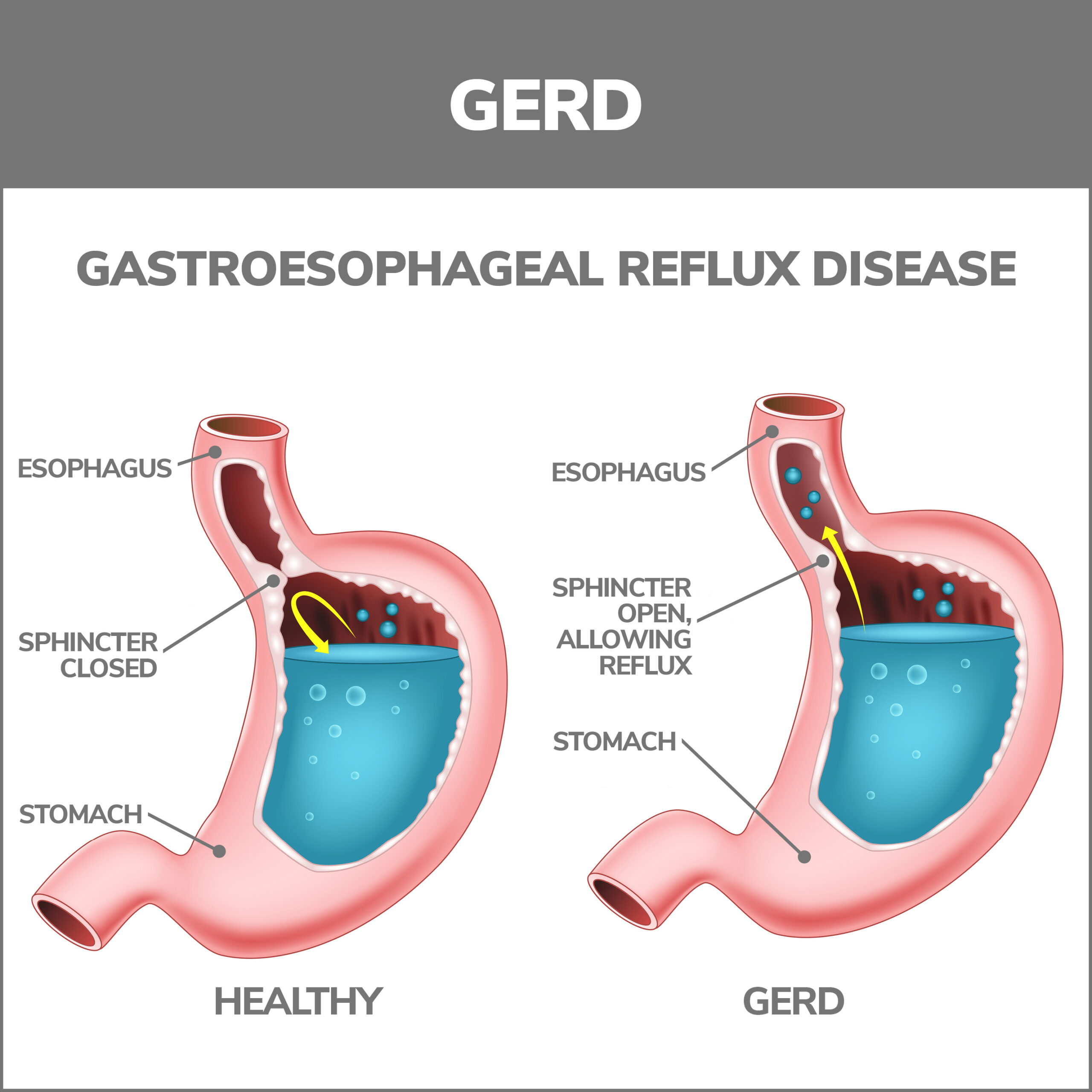
- GERD – GERD, an abbreviation for gastroesophageal reflux disease, occurs when stomach acid backs up into the esophagus. This happens because the lower esophageal sphincter fails to close following digestion. Over time, it results in inflammation of the esophageal lining and damage to surrounding tissues.
- Barrett’s Esophagus – Longstanding GERD can cause Barrett’s Esophagus. As the condition progresses, the cellular structure inside your esophagus changes, damaging and possibly increasing your cancer risk.
- Lower Sphincter Malfunction – This issue, officially called achalasia, occurs when the lower esophageal sphincter fails to open. This prevents food from entering the stomach and disrupts digestion.
- Esophageal Spasms – Spasms are abnormal movements of the esophagus muscles. When severe enough, they prevent the proper flow of food to the stomach.
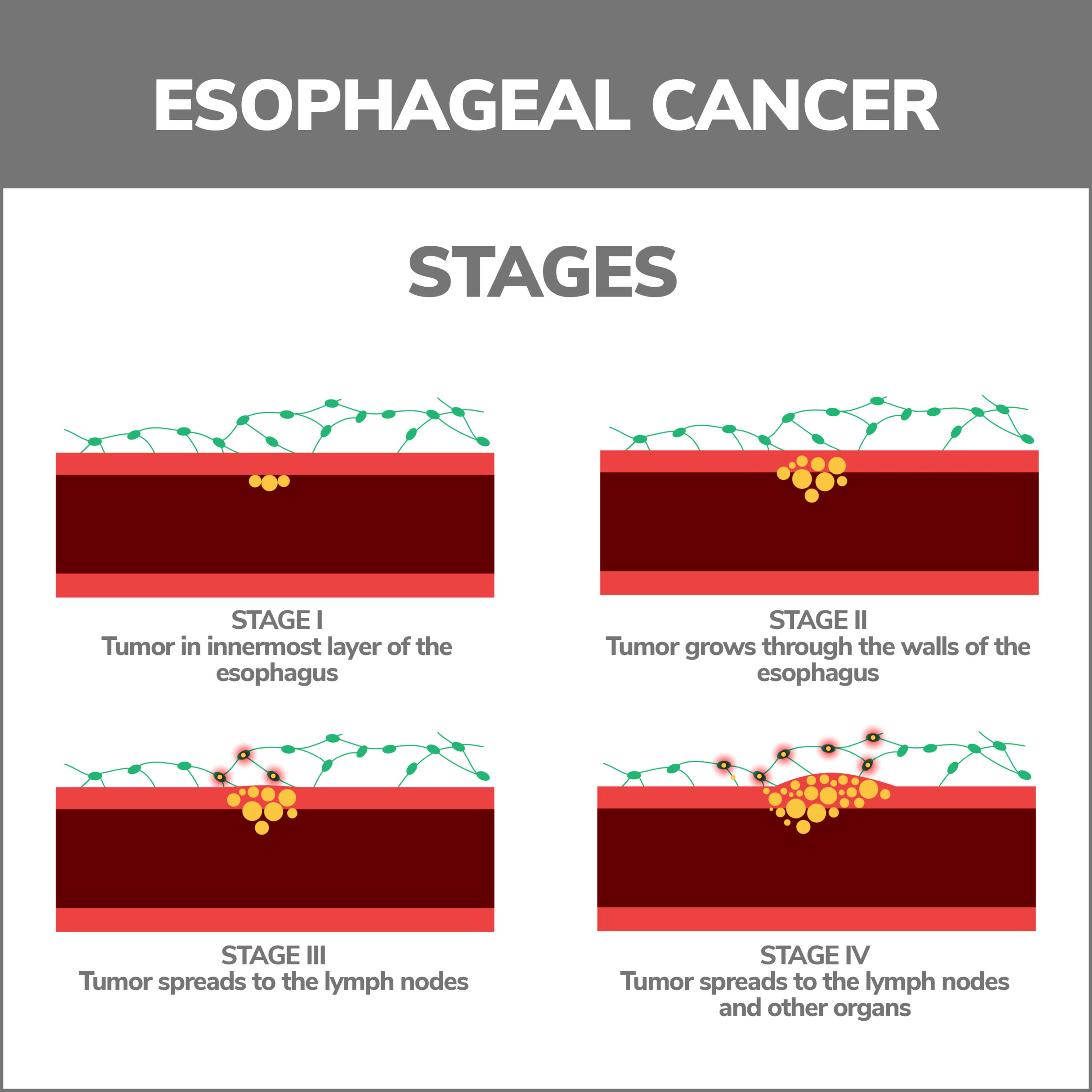
- Esophageal Cancer – When cells in your esophagus grow wildly, it carries the potential for tumor development. Cancer can interfere with digestion and metastasize to other bodily regions if not diagnosed early.
Causes And Risk Factors
The preceding problems might result from one or several causes or risk factors, including:
- Alcohol Intake – Excessive alcohol use irritates and may eventually damage esophageal tissues. Excessive drinking has been linked to potentially serious concerns such as GERD, Barrett’s Esophagus, and esophageal cancer.
- Tobacco Use – Tobacco contains many abrasive chemicals like nicotine. These products can inflame or injure esophageal cells. Like an excessive intake of alcohol, smoking and the inhalation of secondhand smoke have been connected to potentially life-limiting esophageal diseases.
- Dietary Habits – Spicy, highly processed, and frozen foods contain potentially irritating chemicals and preservatives. These materials can also stimulate stomach acid production, which could exacerbate existing esophageal and other digestive conditions.
- Medications – Certain therapeutic drugs may cause or increase your risk of contracting esophageal disorders. Many of these substances contain abrasive or acid-stimulating chemicals.
- Other Causes – Excess body weight associated with obesity and the hormonal changes common during pregnancy have been identified as additional risk factors.
Symptoms
The physical manifestations often vary depending on the specific underlying issue. Esophageal disorders typically produce common symptoms such as:
- Heartburn.
- A persistent dry cough.
- A sore throat.
- Hoarseness.
- Swallowing difficulties.
- Nausea.
- Vomiting.
- Belching.
- Indigestion.
Severer illnesses might produce back, chest, and neck pain, wheezing, and weight loss.
Complications
If not diagnosed early, illnesses like GERD, Barrett’s Esophagus, and cancer could cause extensive esophageal damage rendering digestion challenging, if not impossible. Malnutrition increases your risk of many other sicknesses. Cancer could spread throughout the body, negatively impacting many other systems, and eventually leading to significant disability or death.
Diagnosis
Your doctor uses several diagnostic tests to confirm an esophageal disorder’s presence, including:
- pH Measurement – This test helps gauge the acid concentrations in your esophagus.
- Barium Swallow – You are administered a liquid containing the element barium during this examination. X-rays track the progression of the solution through your esophagus. Disrupted or disjointed flow appearing on the scans can suggest some underlying disorder.
- Endoscopy – Doctors examine your esophagus’s inner workings using a small, thin, camera-equipped device known as an endoscope. It is also fitted with a small incision-making tool enabling them to collect small tissue samples for laboratory study.
- Manometry – This device lets physicians determine how well your esophagus’s muscles perform while swallowing liquids.
Your doctor will also likely subject you to a complete physical examination. Symptoms caused by esophageal problems often mimic those from other issues. They will document and record your vital statistics, followed by questions about when your symptoms began, if any actions worsen them and if you regularly take any medications.
Potential Treatment Options
Factors such as the specific underlying ailment, the condition’s severity, your age, overall health, weight, and the medications you use would determine the treatment your doctor prescribes.
Relatively simple and minor issues might be resolved through efforts like altering your diet, limiting alcohol intake, and not smoking any longer. Changing the dosage or finding a suitable alternative might yield beneficial results if medications are the cause. Medications might limit the symptoms resulting from GERD.
More serious issues such as Barrett’s Esophagus, sphincter damage, or cancer might need aggressive therapies like surgery. Common procedures include the removal of malignant esophageal tissues, esophageal dilation (a balloon is inflated in your esophagus to widen narrow gaps), and stricture-remediating stent placement.
Preventing Esophageal Problems
Not every esophageal disorder can be intercepted. You can reduce your risk by employing preventative measures such as:
- Practicing Healthier Lifestyle Habits – Avoid certain esophageal disorders by consuming nutritious foods, limiting your consumption of spiced and processed foods, remaining adequately hydrated, steering clear of alcoholic and caffeinated foods and beverages, and limiting stress. Increased tension often increases the body’s production of stomach acid, which can worsen existing problems.
- Observing Better Dietary Traits – Observe better eating habits. Consume several smaller meals throughout the day instead of one or two large sittings. Avoid consuming large quantities of food in the hours before bedtime. Avoid lying down period for several hours following a meal.
- Sleeping In a Raised Position – Sleeping with your pillow raised or in a sitting position can prevent acid from backing up into your throat during the nighttime hours.
- Getting Regular Medical Checkups – You should get routine medical screenings. This enables your doctor to identify problems in the earliest possible stage and offer you the most effective treatment options.
Prognosis
Your prognosis hinges on several key concerns, such as:
- The specific disorder.
- How advanced the problem is.
- The impact on your ability to live well and function.
- If you have any co-existing medical issues.
Ailments resulting from easily fixable problems might resolve in a few days. Several issues often need more aggressive therapy. Even the most serious problems can likely be addressed or cured if detected was made as early as possible.
Contacting Us
Please contact us if you have been diagnosed with an esophageal disorder or are currently experiencing the symptoms of a potential problem. Our practice began more than 15 years ago and has emerged as one of the leading gastroenterology practices in central Florida. We perform a host of diagnostic procedures using state-of-the-art equipment in a friendly, comfortable, and inviting atmosphere where patient care is always a top priority. Contact us today!